Radiotherapy
Radiotherapy provides options to care teams treating cancers at various stages and in many cases provides improved outcomes in many cases compared to chemotherapy alone. The value of these contributions is rarely captured and ascribed to radiotherapy.
Value based healthcare would appraise and quantify this, allowing for much more effective use of resources.
Radiotherapy (RT) has evolved to be one of the essential therapies for cancer treatment. It uses photons from X-rays to impact the tumors and destroy its genetic material avoiding its further growth. There are different ways to use RT for cancer treatment:
- Cure - In cases where the tumor is easily located and no metastasis has taken place, the use of RT can reduce the tumor and eliminate it from the body.
- Complement to surgery - After a tumor removal surgery is performed, the area is irradiated in order to remove remaining malign tissue and lower the probability of recurrence.
- Support therapy for chemotherapy - RT is used to reduce the size of the tumor.
- Palliative care - For several types of tumors that cannot be removed or eliminated, RT is used to reduce their size reliving the patient from the symptoms.
Currently three possible types of RT are available: external beam radiation, internal radiation (Brachytherapy) and systemic therapy. The type of radiation used depends on several factors like, the size of the tumor, the type of cancer, location in the body, age of the patient and other possible medical conditions. In order to establish the radiation technique and the radiation dose that are going to be used in each patient, there are several supporting tools that are used:
- Treatment planning systems.
- Radiation therapy simulators.
- Oncology information systems.
- Radiotherapy quality assurance dosimetry equipment.
- Patient positioning verification devices.
RADIOSURGERY
Stereotactic radiosurgery is a form of radiation therapy that focuses gamma rays or x-rays on a small area of the body. Other types of radiation therapy are more likely to affect nearby healthy tissue. Stereotactic radiosurgery better targets the abnormal area.
It is a medical procedure that allows non-invasive treatment. The initial application of radiosurgery was in treatment of lesions in the brain, a technique also known as stereotactic radiosurgery (SRS). In addition to brain tumours, it has also been shown to be beneficial for the treatment of some non-cancerous conditions, including functional disorders such as arteriovenous malformations (AVMs) and trigeminal neuralgia. Leksell Gamma Knife is the most widely used technology for intracranial SRS and is considered the gold standard.
Radiosurgery is also used for tumours in other parts of the body (extracranially). This is known as Stereotactic Body Radiation Therapy (SBRT) and is a treatment procedure similar to SRS. A stereotactic radiation treatment for the body means that a specially designed coordinate-system is used for the exact localisation of the tumours in the body to deliver a single high dose radiation treatment or a few fractionated radiation treatments (usually up to 5 treatments). A high potent biological dose of radiation is delivered to the tumour, improving the cure rates for the tumour, in a manner previously not achievable by standard conventional radiation therapy.
Stereotactic radiosurgery of the brain and spine is typically completed in a single session. Body radiosurgery is used to treat lung, liver, adrenal and other soft tissue tumors, and treatment typically involves multiple (three to five) sessions.
EXTERNAL BEAM RADIATION
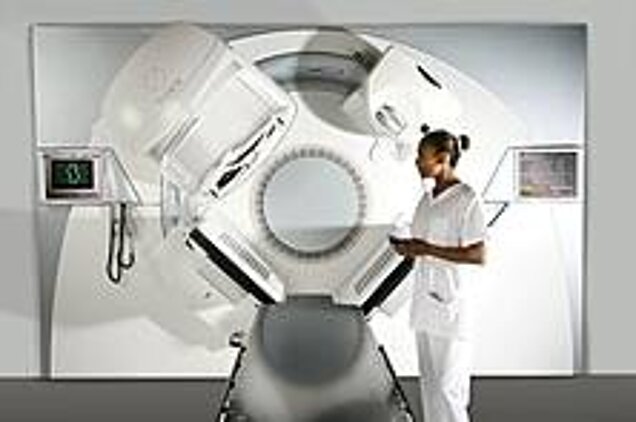
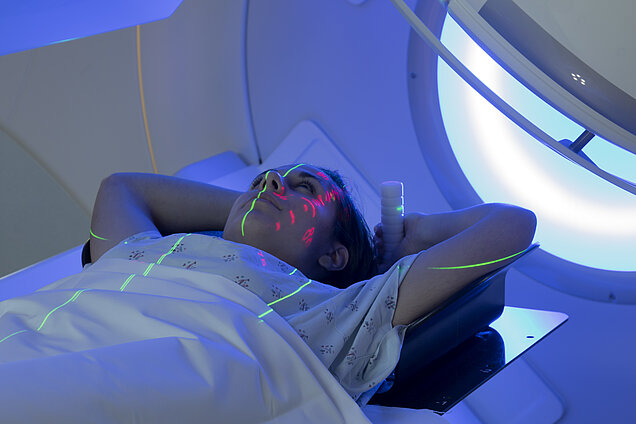
External beam radiation was the first type of RT ever developed. It uses a source of X-ray or gamma ray beams directed to the patient, who is positioned in front of the radiation source a few centimetres away. The equipment used for this therapy is called Linear Particle Accelerator (LINAC). To avoid damage to surrounding tissue, before starting the therapy a simulation is performed, in order to calculate the amount of radiation that is needed to achieve the best therapy result using as less radiation as possible.
Examples of External-beam radiation therapy devices:
- Ionizing radiation accelerators using X-rays and gamma rays using different treatment procedures (3-D CRT, IGRT, IMRT, SBRT, IMAT)
- Ionizing radiation accelerators using charged particles (electron beams, proton beams, Carbon Therapy)
PROTON THERAPY
Proton therapy is one of the possible forms of external beam radiation therapy, in which instead of X-ray or gamma ray, which are photon emissions, protons emissions are used as a source of radiation. The advantage of using this radiation is that the way protons release their energy will affect less the surrounding tissue and have a bigger effect on the objective planed in the simulation. This will allow to use a higher amount of radiation in the RT without endangering the patient’s health. With the advantages, proton therapy is mainly used when the tumor is close to an important healthy structure of the patient, for example brain tumors or prostate cancer.
NUCLEAR MEDICINE
Nuclear Medicine examinations are used for both diagnosis and therapeutic reasons. In Nuclear Medicine diagnosis, metabolic processes are made visible by administering radioactive pharmaceuticals to patients via skin injection, in tablet form or by inhalation. These substances accumulate in certain parts of the body where they render metabolic processes visible.
In Nuclear Medicine therapy, special radiation with short-range effects is used. The substances administered reach the diseased cells and destroy them by radioactive radiation. The best-known example of this is radioiodine therapy for thyroid patients.
A comprehensive tool was developed by AIPES to get familiar with nuclear medicine. Click here for more information
INTERNAL BEAM RADIATION (BRACHYTHERAPY)
Internal beam radiation is a therapy performed inside the body, directly to the tumor. There are two possibilities of this kind of therapy: low dose rate and high dose rate therapy.
The lower dose therapy is performed by implanting the radiation source in the body of the patient; the radiation energy source will decay on time, while radiating the tumor with its energy. At the end of the therapy, the source can be left in the body since it has no harm after the radiation is finished.
The high dose radiation therapy consists on planting a temporary catheter in order to reach the tumor and provide a direct radiation to the tissue, removing the source at the end of the session. The internal beam radiation therapy can be used in combination with an external beam radiation therapy to boost up the speed of the therapy.
SYSTEMIC RADIATION THERAPY
In systemic radiation therapy, nuclear medicine is used to give the patient a dose of a radioactive substance, combined with a specific antibody, in order for the substance to travel to the blood stream and thanks to the antibody, attach to the specific cancer cells and radiate them with the radioactive substance. This therapy is mainly used for thyroid cancer due to its affinity to Iodine.